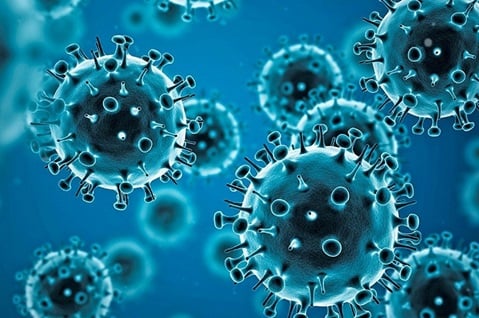
In a significant departure from federal CDC guidelines, California and Oregon have recently revised their COVID-19 isolation policies, breaking away from the recommendations provided by the US Centers for Disease Control and Prevention (CDC). These states, traditionally known for their cautious approach to pandemic policies, are now setting a new precedent by allowing individuals who test positive for COVID-19 to forego a set isolation period. Even those without symptoms are no longer obligated to isolate at all.
This shift in policy marks a departure from the CDC’s guidance, which advocates for a minimum isolation period of five days for individuals with COVID-19. California and Oregon, however, argue that their decisions are grounded in the changing landscape of the pandemic, with increased vaccination coverage, natural immunity, and the availability of effective treatments.
Dr. Tomás Aragón, the director of the California Department of Public Health, provided insight into the reasoning behind the change, stating, “Our policies and priorities for intervention are now focused on protecting those most at risk for serious illness while reducing social disruption that is disproportionate to recommendations for the prevention of other endemic respiratory viral infections.”
While the CDC emphasizes a minimum isolation period of five days due to the heightened infectiousness during that time, California and Oregon contend that the evolving situation, with reduced severe impacts, justifies the alteration in policy. It’s important to note, however, that the scientific understanding of infectious periods remains consistent with the CDC’s recommendations.
Oregon took the first step in this direction, adjusting its isolation policy in May following the lifting of the COVID-19 public health emergency. California followed suit earlier this month. Data from Oregon suggests that the policy change has had minimal effects on virus trends, with hospitalization rates and emergency department visits remaining below the national average.
Public health experts acknowledge that the decision to revise isolation policies involves weighing trade-offs and considering evolving social norms and workplace pressures. Jennifer Nuzzo, an epidemiology professor at Brown University School of Public Health, commented on the situation, saying, “I don’t think this is reflecting updated science, but this is reflecting changing social norms and increasing workplace crunches.”
Despite concerns about potential impacts on community transmission, some experts argue that stricter isolation policies might have unintended negative effects on public health. Dr. Sarita Shah, an infectious disease epidemiologist at Emory University, highlighted the reluctance of individuals to get tested due to fear of isolation repercussions, which might be alleviated with less restrictive policies.
Equity considerations also played a role in Oregon’s decision to revise its isolation policy. Dr. Dean Sidelinger, Oregon’s state health officer, emphasized the need to avoid unnecessary burdens on families, keeping children out of school, and limiting people’s access to work.
The CDC, while noting its ongoing evaluation of the latest data, acknowledges the authority of local jurisdictions to shape health guidelines based on their specific situations. The changes in California and Oregon align their COVID-19 isolation policies more closely with the management of other respiratory viruses, emphasizing the use of tests as a tool rather than a penalty.
As the ongoing debate continues regarding the balance between mitigating the impact of COVID-19 and minimizing social disruption, public health experts emphasize the importance of individualized health decisions and discussions between individuals and healthcare providers. The evolving risk-benefit balance in light of advancements in managing COVID-19 calls for continued conversation and debate.
While the severity of outcomes for COVID-19 has decreased over the years, the latest CDC data shows that COVID-19 hospitalization rates have consistently been at least twice as high as they’ve been for the flu this respiratory virus season. Thousands of people have died from COVID-19 in the first two weeks of this year, highlighting the ongoing burden of disease.
Despite the ongoing burden, tools available to manage COVID-19 have evolved rapidly and are much more in line with what’s available to manage other respiratory diseases, experts say. Isolation is just one strategy, and California and Oregon still encourage people who test positive to wear a mask for at least 10 days.
Also, the policy changes in these states offer a broad, population-level approach to COVID-19 management. However, individuals and places like hospitals may adjust based on their own risk tolerance.
“Health decisions generally are individual. At the end of the day, you’re always having that discussion with your doctor about what’s going to be best for you,” Shah said. The same internal analysis has now been happening around COVID-19 for years, and the risk-benefit balance may have shifted for many people.
“I think it’s time to have that conversation and to have that debate.”